
For the last decade, the Contraceptive Security Indicators (CSI) Survey has collected, monitored and analyzed data from around the world to share collective insight about contraceptive security: the ability to reliably choose, obtain and use a wide range of high-quality and affordable family planning (FP) methods.
While the survey and its findings address many critical components driving global contraceptive security, the indicators related to Universal Health Coverage (UHC) may be the most important. After all, contraceptives can only be utilized if they are accessible to those who need them.
Increase in Popularity of Implants
Data from Demographic Health Surveys (DHS) show increasing modern contraceptive prevalence rates (mCPR) and/or decreasing rates of unmet need. An important factor driving these rates is the dramatically rising popularity of long-acting contraceptive implants because of price reductions, increased supply and other factors.
The prevalence rate of implants in sub-Saharan Africa was only 1.1 percent in 2011, but by 2018 implant use in Burkina Faso, Senegal, Ghana, Kenya and the Democratic Republic of the Congo accounted for one-fourth to one-half of all modern method use in those countries, according to a study by IntraHealth International.
Popularity of implants has also risen during the COVID-19 pandemic when lockdowns have impeded access to clinics or women feared frequenting them because of the virus. Women opted for longer-acting contraception instead of shorter-acting contraceptives like pills. The UN Population Fund estimated that lockdowns would prevent 13 to 51 million women in lower and middle-income countries from accessing modern contraceptives, leading to an additional 325,000 to 15 million unintended pregnancies, depending on the level of health service disruption.
Health Care Workers Need Focused Training
Another factor contributing to increased use of implants is the wider adoption of high-impact service delivery practices. But it is unclear, especially with diversion of focus and funds to COVID-19, that expansion of these practices will keep pace with the demand for implants. Implants and intrauterine devices require access to a trained health care provider—critical to UHC and often unavailable in rural or hard-to-reach areas.
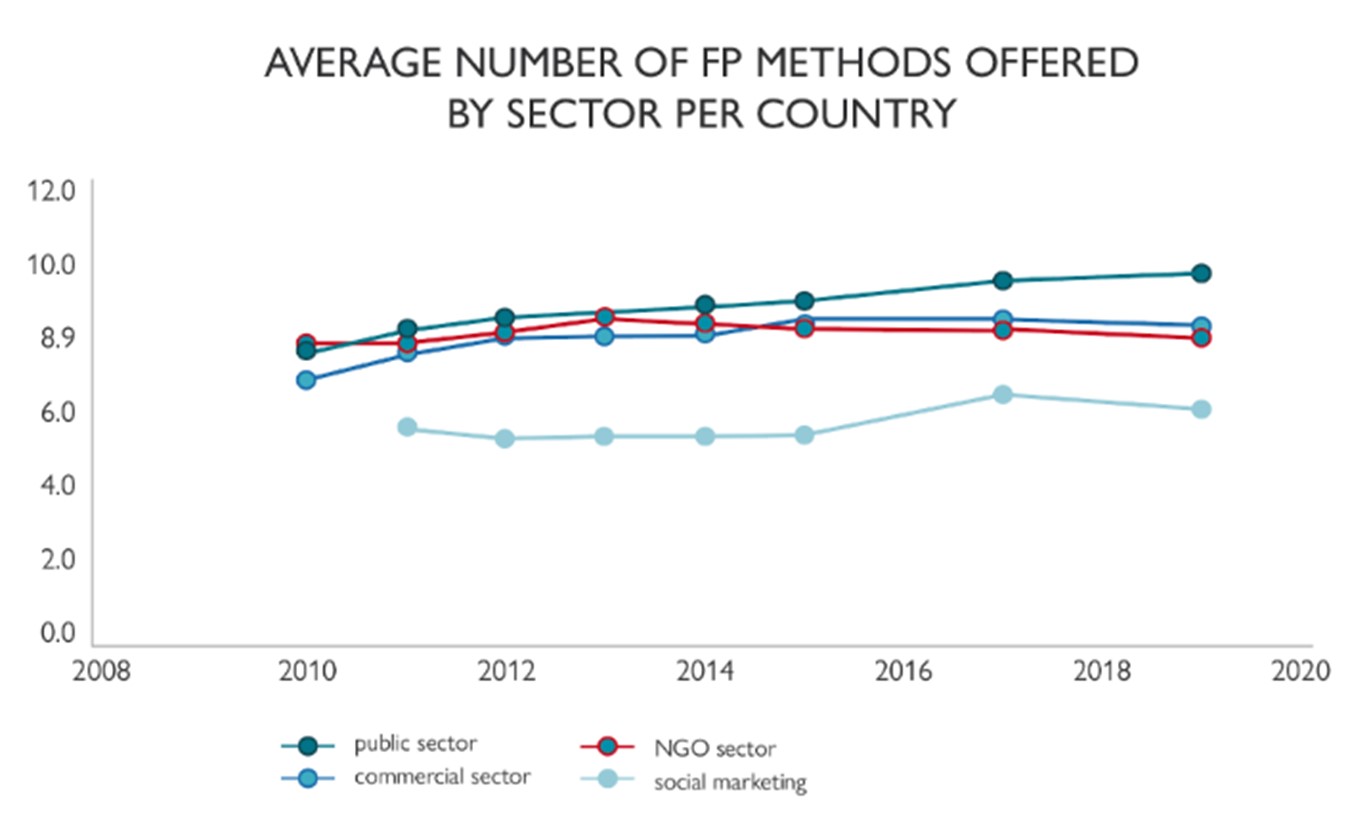
It is also important to note that while each of the CSI surveyed countries relies on the partnership of multiple sectors to meet its contraceptive needs, the public sector provides the most comprehensive suite of FP methods. The range of products within this sector appears to be expanding faster than others (Figure 1).
Each of the CSI surveyed countries, relying on a multi-sectoral partnership, identified an approximate range of how many public sector FP providers at the national level had the necessary training in implant and intrauterine devices insertion and removal. As the below Figure 2 shows, few countries were in the 60-100 percent range.
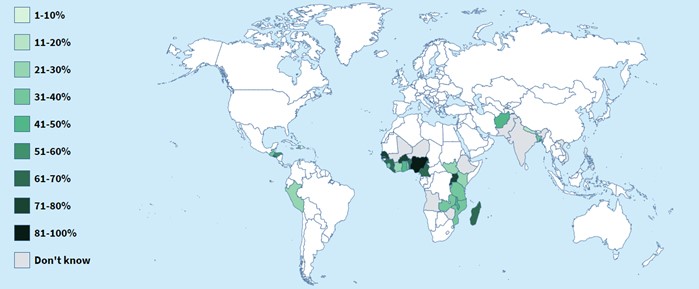
Discriminatory Practices Hinder Access
Another impediment to UHC as it relates to FP is discrimination. While many of the surveyed countries reported policies crafted specifically to prevent this and provide universal access to contraceptives and services, some nations place burdens on access by minors or unmarried youth. Societal pressure also plays a large part in discouraging availability of FP for these populations.
Within the countries that have established access to a wide range of reproductive health products for all as a fundamental human right, improving UHC and removing barriers to access may be a pivotal step toward meeting key goals. Data collected from over 40 countries in the last decade demonstrates there is room for improvement in the public sector’s FP services and medical expertise and removing policies that bar sub-populations from accessing critical reproductive health services.
For more details on the link between CSI and UHC, please see our technical brief.
By assisting countries in gathering and tracking data to improve access to FP methods, the CSI Survey contributes new insights into FP and the reproductive health knowledge base. Key findings, raw data, interactive dashboards and other resources are available on the CSI Survey Landing Page.
Authored by Lauren Pell, Quality Management Associate, with GHSC-PSM and Suzanne Gold, Monitoring and Evaluation Specialist with GHSC-PSM.